Insomnia
Why You Aren't Sleeping and What to Do About it
Insomnia is not simply “not sleeping well.” It is a disruption of the brain’s carefully coordinated sleep–wake system. For some, it means lying awake for hours. For others, it means waking repeatedly through the night. For many, it’s both.
Clinically, insomnia is defined as difficulty initiating sleep, maintaining sleep, or waking too early — accompanied by daytime impairment (fatigue, irritability, poor concentration, low mood, decreased performance).
Let’s break this down systematically.
The Three Main Types of Insomnia
1) Trouble Falling Asleep (Sleep-Onset Insomnia)
4
What it looks like:
Takes more than 30–45 minutes to fall asleep
Racing thoughts at bedtime
“Second wind” late at night
Anxiety about not sleeping
Most common causes:
Hyperarousal (stress, anxiety, rumination)
Elevated evening cortisol
Blue light exposure from screens
Late caffeine intake
Shifted circadian rhythm (night owls)
Perimenopause / hormonal fluctuations
Stimulant medications
Most likely effective treatments:
Cognitive Behavioral Therapy for Insomnia (CBT-I)
Strict wind-down routine
Melatonin (low dose, 0.3–1 mg)
Magnesium glycinate
Glycine
Limiting screens 60–90 minutes before bed
Consistent sleep/wake time
2) Trouble Staying Asleep (Sleep-Maintenance Insomnia)
4
What it looks like:
Waking multiple times per night
Waking at 2–4 AM and unable to return to sleep
Light, fragmented sleep
Most common causes:
Elevated nighttime cortisol
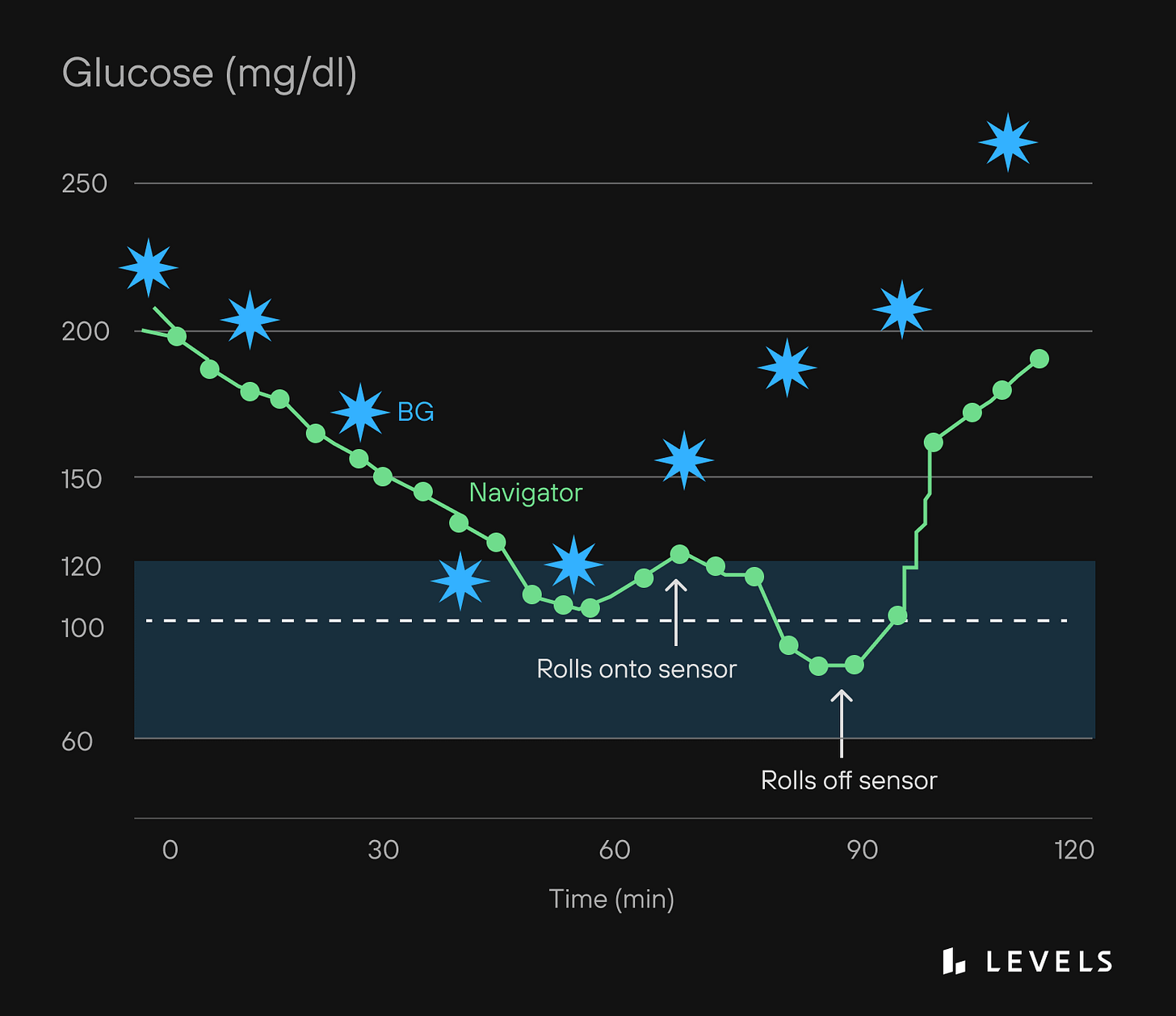
Blood sugar dips (reactive hypoglycemia)
Sleep apnea
Alcohol before bed
Hormonal changes (especially low progesterone or estrogen)
Chronic pain
Enlarged prostate (in men)
Depression (early morning awakening)
Most likely effective treatments:
Evaluate for sleep apnea
Stabilize evening blood sugar (protein + fat snack if needed)
Reduce alcohol
Address pain
Progesterone (when clinically appropriate)
Adaptogens (ashwagandha, phosphatidylserine for high cortisol)
3) Combined Insomnia (Onset + Maintenance)
4
What it looks like:
Difficulty falling asleep
Multiple awakenings
Non-restorative sleep
Daytime exhaustion
Common underlying drivers:
Chronic stress
Long-standing anxiety disorder
Hormonal dysregulation
Circadian rhythm disruption
Poor sleep hygiene
Overtraining or overwork
These patients often require a multi-layered approach.
What’s Happening in the Brain During Sleep?
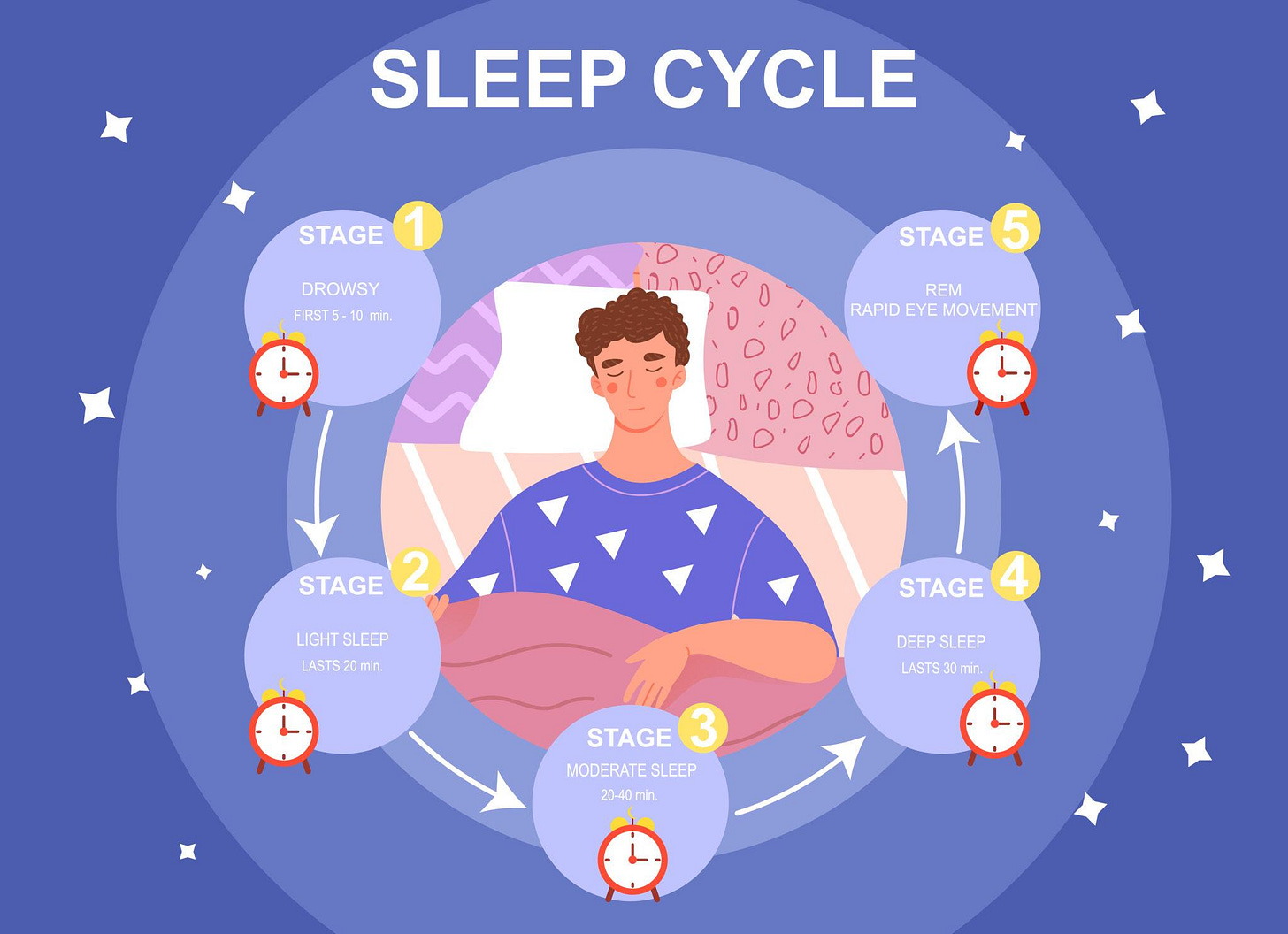
Sleep occurs in cycles (~90 minutes) that include:
Stage 1: Light sleep
Stage 2: Stable sleep
Stage 3 (Deep Sleep / Slow Wave Sleep): Physical restoration, growth hormone release
REM Sleep: Memory consolidation, emotional processing
4
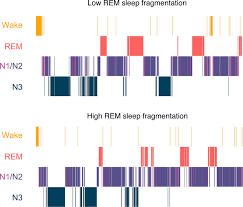
When Sleep Stages Are Disrupted
Reduced deep sleep: muscle aches, fatigue, immune weakness
Reduced REM: irritability, anxiety, poor emotional regulation
Frequent awakenings: poor memory, brain fog
Short total sleep time: increased cardiovascular risk, insulin resistance, weight gain
Chronic insomnia shifts the autonomic nervous system toward sympathetic (“fight or flight”) dominance.
Sleep Hygiene: The Foundation
Sleep hygiene is not glamorous, but it works.
Non-negotiables:
Same bedtime and wake time (even weekends)
No screens 60–90 minutes before bed
Cool bedroom (60–67°F)
Total darkness (blackout curtains)
No caffeine after noon
Avoid alcohol within 3 hours of bed
No heavy meals late
Get morning sunlight exposure
Exercise — but not intensely right before bed
Bed is for sleep and intimacy only
Small violations, done repeatedly, equal chronic insomnia.
Treatment of Insomnia
1) Conventional Medical Treatments
CBT-I (gold standard)
Short-term sedative medications (cautious use)
Low-dose trazodone
Doxepin
Suvorexant / orexin antagonists
Medication may help short-term, but behavioral correction is more durable.
Natural and Integrative Approaches
For patients who prefer a conservative or complementary strategy, here are structured options.
Special Frequency Music
4
Some individuals respond to:
Binaural beats
432 Hz or 528 Hz music
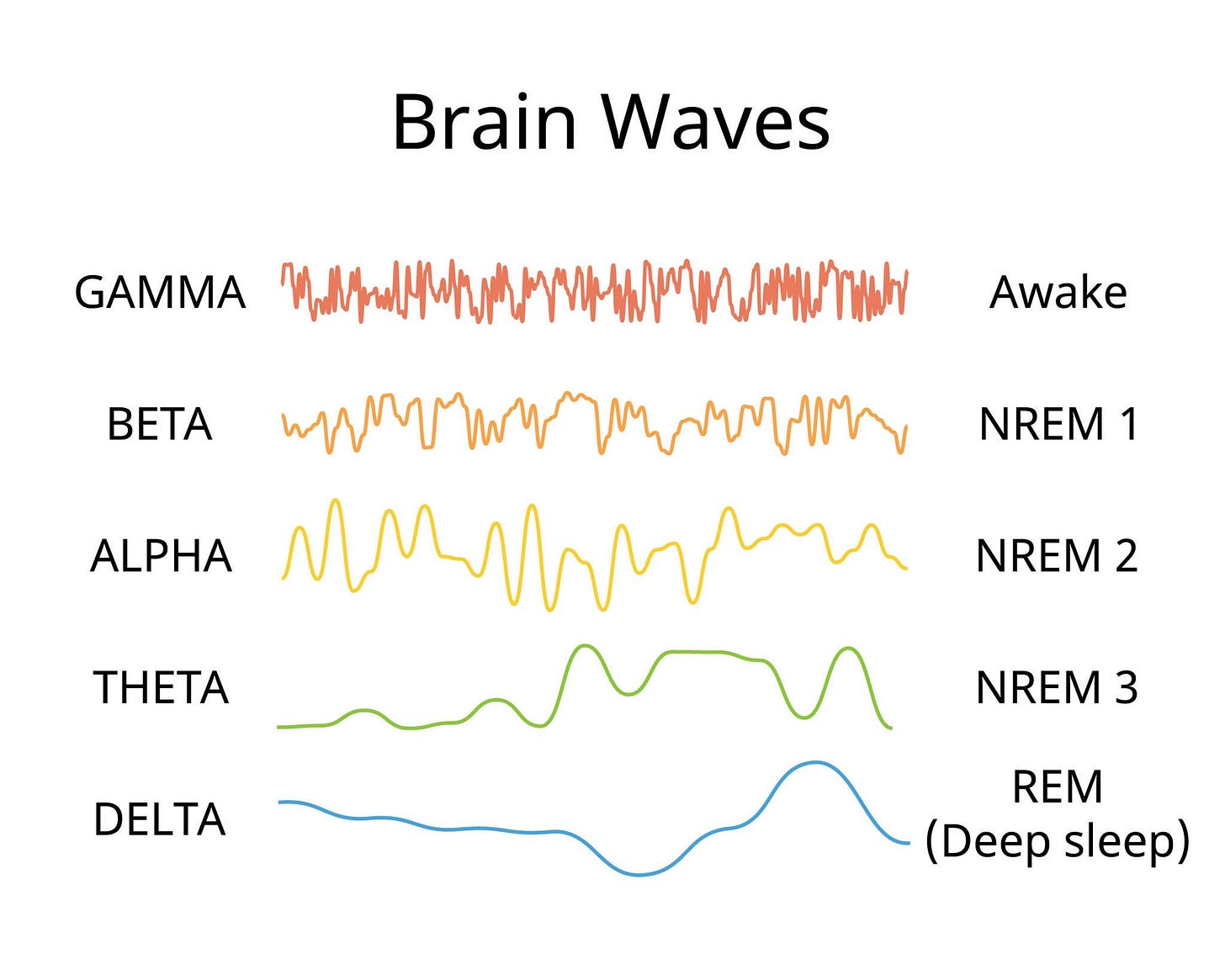
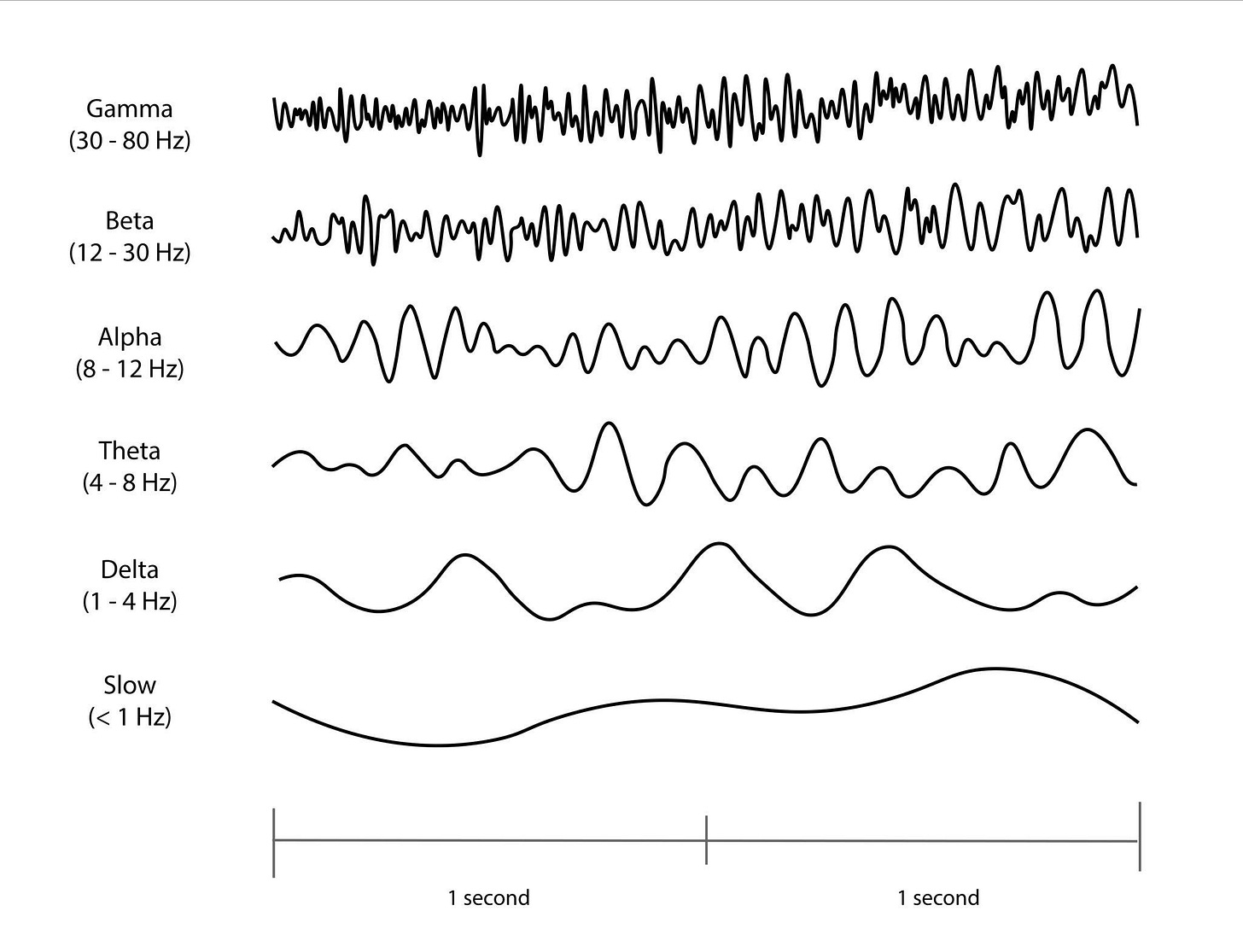
Delta wave entrainment tracks (0.5–4 Hz)
The theory: certain frequencies promote parasympathetic dominance and slower brain waves. Evidence is mixed but promising for relaxation and anxiety reduction.
Natural Supplements (Evidence-Informed)
Magnesium glycinate or threonate
Melatonin (low dose preferred)
L-theanine
Glycine (3 grams at bedtime)
Ashwagandha
Phosphatidylserine (for high nighttime cortisol)
Valerian root
Passionflower
5-HTP (careful if on SSRIs)
These should be tailored to the type of insomnia.
Essential Oils
4
Most commonly used:
Lavender
Roman chamomile
Cedarwood
Bergamot
Mechanism: limbic system calming via olfactory pathways.
Best used via diffuser 30–60 minutes before bed.
Homeopathic Remedies
Homeopathy is individualized. Common remedies used for insomnia include:
Coffea cruda – racing thoughts
Nux vomica – stress, business-minded overdrive
Arsenicum album – anxiety at night
Ignatia – grief-related insomnia
Clinical evidence varies, but some patients report benefit when matched appropriately.
A Practical Strategy
If you are struggling with insomnia:
Fix sleep hygiene first.
Identify which type you have.
Correct circadian rhythm.
Address stress physiology.
Layer in natural supports if needed.
Consider CBT-I if persistent.
Screen for sleep apnea when indicated.
Insomnia is rarely random. It is usually a signal — hormonal, neurological, metabolic, psychological, or behavioral.
Correct the root cause, and sleep often follows.
Supplement Protocol for Insomnia
A subtype-specific, mechanism-based approach
Insomnia is not one condition. The supplement strategy should match the physiology driving the sleep disruption. Below is a structured, practical protocol organized by subtype.
1️⃣ Sleep-Onset Insomnia
(Difficulty falling asleep / racing mind / hyperarousal)
Most Likely Mechanisms
Elevated evening cortisol
Sympathetic overactivation
Rumination / anxiety
Delayed circadian rhythm
Screen/light exposure
Primary Supplement Strategy
Core Stack (Start Here)
Magnesium glycinate
200–400 mg 60 minutes before bed
Calms NMDA excitability, supports GABA
L-theanine
100–200 mg at bedtime
Promotes alpha-wave relaxation
Low-dose melatonin
0.3–1 mg 2 hours before desired bedtime
Helps phase-shift circadian rhythm
If Racing Thoughts Persist
Glycine
3 grams at bedtime
Lowers core body temperature, improves sleep latency
Phosphatidylserine (if elevated nighttime cortisol suspected)
100–300 mg at dinner
Ashwagandha (KSM-66 or Sensoril)
300–600 mg in evening
Reduces stress reactivity
If Delayed Sleep Phase (Night Owl Pattern)
Morning bright light exposure
Melatonin 0.3 mg 3 hours before bedtime
Strict wake time
2️⃣ Sleep-Maintenance Insomnia
(Waking at 2–4 AM / fragmented sleep)
4
Most Likely Mechanisms
Cortisol spike
Blood sugar drop
Hormonal shifts (low progesterone, perimenopause)
Alcohol effect
Mild sleep apnea
Primary Supplement Strategy
Core Stack
Magnesium glycinate
200–400 mg at bedtime
Glycine
3 grams at bedtime
Protein + fat snack before bed (if hypoglycemia suspected)
Almond butter
Greek yogurt
Small handful of nuts
If 3 AM Cortisol Spike Pattern
Phosphatidylserine
200–300 mg with dinner
Ashwagandha
300–600 mg evening
Relora (Magnolia + Phellodendron)
250–500 mg evening
If Perimenopausal / Low Progesterone Pattern
Discuss bioidentical progesterone when appropriate
Consider:
Magnesium
Vitamin B6 (25–50 mg)
Black cohosh (short-term use)
If Suspected Sleep Apnea
Supplements will not correct airway obstruction.
Recommend formal evaluation.
3️⃣ Combined Insomnia (Onset + Maintenance)
4
Most Likely Mechanisms
Chronic stress physiology
Long-term hyperarousal
Hormonal dysregulation
Poor sleep hygiene layered with anxiety
Structured Multi-Layer Approach
Phase 1 (Weeks 1–2): Nervous System Reset
Magnesium glycinate 300–400 mg
L-theanine 200 mg
Glycine 3 g
Phosphatidylserine 200 mg with dinner
Phase 2 (If Needed)
Add:
Melatonin (low dose)
0.3–1 mg
Valerian root
300–600 mg standardized extract
Passionflower extract
300–500 mg
Phase 3 (Persistent Hyperarousal)
Consider:
5-HTP (50–100 mg at bedtime)
⚠ Avoid if on SSRIs
GABA (100–300 mg)
Variable response; some benefit
Additional Natural Adjuncts
Special Frequency Music
4
Delta wave entrainment (0.5–4 Hz)
Binaural beats
432 Hz or 528 Hz calming tracks
Use 20–40 minutes before sleep.
Essential Oils
4
Lavender
Roman chamomile
Cedarwood
Bergamot
Diffuse 30–60 minutes before bed.
Safety Considerations
Avoid combining multiple serotonergic agents
Use melatonin in physiologic doses (higher is not better)
Evaluate medications that may worsen sleep
Screen for sleep apnea when indicated
Address alcohol use
A Practical Clinical Algorithm
Identify subtype
Correct sleep hygiene
Address cortisol pattern
Stabilize blood sugar
Support GABAergic tone
Add circadian support if needed
Escalate cautiously
Bottom Line
Sleep supplements work best when:
They match the physiology
They are layered intentionally
They are combined with behavioral correction
Insomnia is often a stress regulation disorder — not simply a “lack of sleep problem.”
Dr. P





















https://thedodowsleep.com/
this is a pretty cool device that helps "lead you to fall asleep)